New Manchester partnership
Stopping breast cancer in its tracks, despite coronavirus
Coronavirus is disproportionately affecting cancer patients, whose immunity is low making them more susceptible to the virus. In addition, surgical treatment has had to be postponed for many. The pandemic has also understandably focused charitable spending towards tackling the direct impacts of the virus. However, cancer is not waiting for coronavirus to go away, and patients need support more than ever.
At Action Against Cancer, we have seen a marked drop in income in recent months due to the pandemic. Despite this we are determined to meet the commitments we had planned to fund life-saving research. This includes support for a new key priority project to be undertaken in partnership with The University of Manchester, the Manchester Breast Centre, the Outreach Research and Innovation Group and The Christie Hospital, one of the largest cancer treatment centres of its kind in Europe. We are delighted to announce this new partnership.
This innovative project aims to help patients with HER2+ type breast cancer whose tumours are not responding to treatment, by stopping their cancer in its tracks. Of the 55,200 or so new breast cancer cases diagnosed in the UK each year, more than 6,600 (12%) are HER2+.
Project objectives
Many patients diagnosed with breast cancer are given treatment to shrink a tumour as a first step, before the main treatment, which is usually surgery.
This initial treatment is called “neoadjuvant,” and whilst this is very helpful for some patients, unfortunately it does not work effectively in up to half of HER2+ breast cancer cases. This project aims to understand why this is, assess new drugs in lab models, and then with this knowledge design new clinical trials to test the effect of certain drugs with these patients to see what will work best.
Project outline
The team of scientists plan to analyse residual tumour samples from HER2+ breast cancer patients to discover the “signalling pathways” that remain active and drive the cancer. This can be thought of as similar to a train travelling to its destination through a number of stations. At most of the stations the signalling technology works flawlessly and there are no problems. However, if one signal has a fault, the train can go on the wrong track leading to tragedy.
A signalling pathway is a series of chemical reactions in which a group of molecules in a cell work together to control an outcome, for example cell division or cell death. After the first molecule in the pathway receives a signal, it activates another molecule, and so on until the cell function is carried out. Abnormal activation of signalling pathways can lead to cancer, and conversely, drugs targeting specific molecules in the pathway may help keep cancer cells from growing.
The three-year research project aims to identify the faulty signals and to design new clinical trials at The Christie to test drugs that would keep the patients health on track.
Project team
The team are ideally placed to do this research in terms of relevant expertise and access to key resources. The Manchester Cancer Research Centre Biobank has agreed to provide a wealth of the necessary samples to the team.
Professor Rob Clarke, Professor of Breast Biology at the University of Manchester
- Professor Clarke’s team are highly experienced in generating the types of models of breast cancer as planned in this project.
- Described by one of the scientific peer reviewers for this project as: “among the few scientists around that could tackle this challenge.”
Professor Andrew Wardley, Consultant in Medical Oncology and Medical Director of NIHR Manchester Christie Research Facility
- Chair of the National Cancer Research Institute Breast Cancer Research Group.
- Highly regarded Breast Medical Oncologist, treating patients and leading breast cancer trials at The Christie, in the UK and internationally for 19 years.
- Clinical Director of the Christie hospital Early Phase Trials Unit since 2011.
Patients with treatment resistant HER2+ breast cancer are currently underserved with treatment options and their life prospects are too often bleak. Please support us to change this by donating to Action Against Cancer today.
Back to 'News and Events' main menu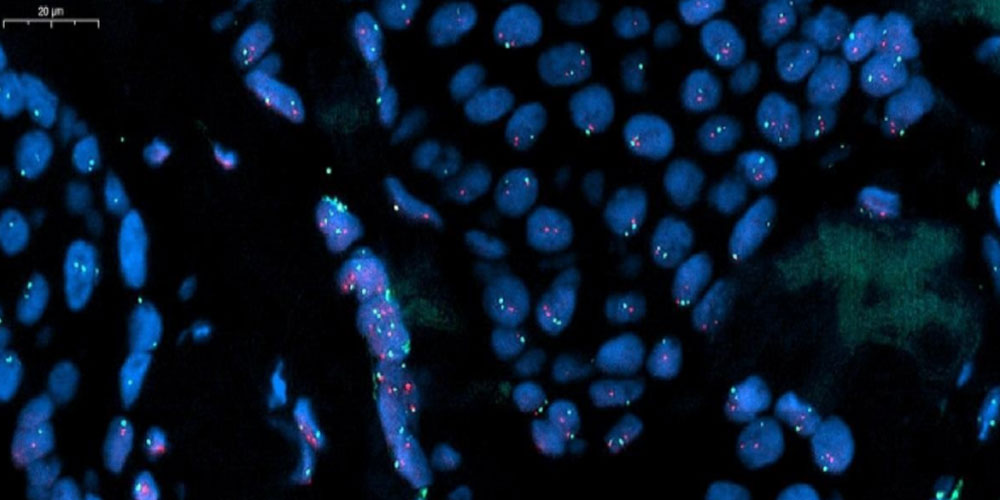




Other News and Events

Celebrities support AAC!
Action Against Cancer Ambassadors Julian and Cat O'Dell's live music fundraiser event Catfest has been a huge success over the past few years... Read more
Fundraise from your Facebook page!
You can now raise vital funds for life saving research right from your Facebook page. This is a really effective way to fundraise and is super easy... Read more
Big step closer to new drug
One of the first projects Action Against Cancer funded after establishing as a charity in 2011 resulted in the discovery of a cancer... Read more
